2 results
Factors associated with SARS-CoV-2 and community-onset invasive Staphylococcus aureus coinfection, 2020
- Kelly Jackson, Sydney Resler, Joelle Nadle, Susan Petit, Susan Ray, Lee Harrison, Ruth Lynfield, Kathryn Como-Sabetti, Carmen Bernu, Ghinwa Dumyati, Marissa Tracy, William Schaffner, Holly Biggs, Isaac See
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 3 / Issue S2 / June 2023
- Published online by Cambridge University Press:
- 29 September 2023, pp. s84-s85
-
- Article
-
- You have access Access
- Open access
- Export citation
-
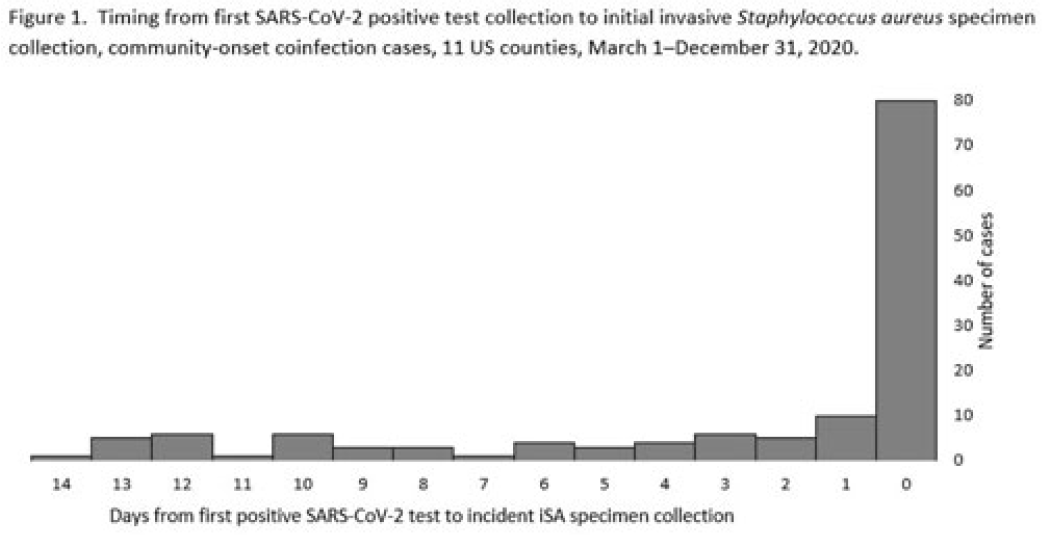
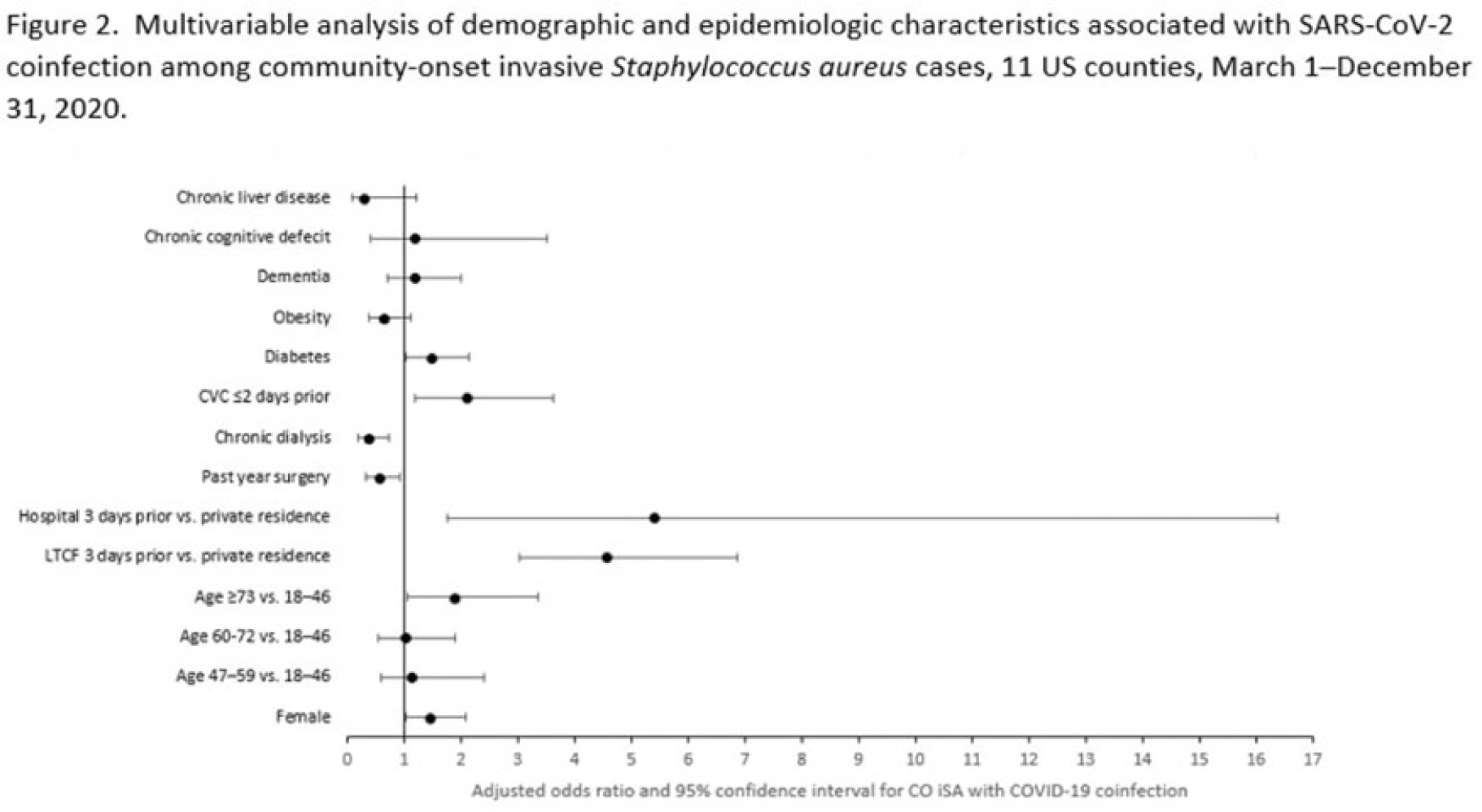
Background: Previous analyses describing the relationship between SARS-CoV-2 infection and Staphylococcus aureus have focused on hospital-onset S. aureus infections occurring during COVID-19 hospitalizations. Because most invasive S. aureus (iSA) infections are community-onset (CO), we characterized CO iSA cases with a recent positive SARS-CoV-2 test (coinfection). Methods: We analyzed CDC Emerging Infections Program active, population- and laboratory-based iSA surveillance data among adults during March 1–December 31, 2020, from 11 counties in 7 states. The iSA cases (S. aureus isolation from a normally sterile site in a surveillance area resident) were considered CO if culture was obtained <3 days after hospital admission. Coinfection was defined as first positive SARS-CoV-2 test ≤14 days before the initial iSA culture. We explored factors independently associated with SARS-CoV-2 coinfection versus no prior positive SARS-CoV-2 test among CO iSA cases through a multivariable logistic regression model (using demographic, healthcare exposure, and underlying condition variables with P<0.25 in univariate analysis) and examined differences in outcomes through descriptive analysis. Results: Overall, 3,908 CO iSA cases were reported, including 138 SARS-CoV-2 coinfections (3.5%); 58.0% of coinfections had iSA culture and the first positive SARS-CoV-2 test on the same day (Fig. 1). In univariate analysis, neither methicillin resistance (44.2% with coinfection vs 36.5% without; P = .06) nor race and ethnicity differed significantly between iSA cases with and without SARS-CoV-2 coinfection (P = .93 for any association between race and ethnicity and coinfection), although iSA cases with coinfection were older (median age, 72 vs 60 years , P<0.01) and more often female (46.7% vs 36.3%, P=0.01). In multivariable analysis, significant associations with SARS-CoV-2 coinfection included older age, female sex, previous location in a long-term care facility (LTCF) or hospital, presence of a central venous catheter (CVC), and diabetes (Figure 2). Two-thirds of co-infection cases had ≥1 of the following characteristics: age > 73 years, LTCF residence 3 days before iSA culture, and/or CVC present any time during the 2 days before iSA culture. More often, iSA cases with SARS-CoV-2 coinfection were admitted to the intensive care unit ≤2 days after iSA culture (37.7% vs 23.3%, P<0.01) and died (33.3% vs 11.3%, P<0.01). Conclusions: CO iSA patients with SARS-CoV-2 coinfection represent a small proportion of CO iSA cases and mostly involve a limited number of factors related to likelihood of acquiring SARS-CoV-2 and iSA. Although CO iSA patients with SARS-CoV-2 coinfection had more severe outcomes, additional research is needed to understand how much of this difference is related to differences in patient characteristics.
Disclosures: None
Excess Costs and Utilization Associated with Methicillin Resistance for Patients with Staphylococcus aureus Infection
- Gregory A. Filice, John A. Nyman, Catherine Lexau, Christine H. Lees, Lindsay A. Bockstedt, Kathryn Como-Sabetti, Lindsey J. Lesher, Ruth Lynfield
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 31 / Issue 4 / April 2010
- Published online by Cambridge University Press:
- 02 January 2015, pp. 365-373
- Print publication:
- April 2010
-
- Article
- Export citation
-
Objective.
To determine differences in healthcare costs between cases of methicillin-susceptible Staphylococcus aureus (MSSA) infection and methicillin-resistant S. aureus (MRSA) infection in adults.
Design.Retrospective study of all cases of S. aureus infection.
Setting.Department of Veterans Affairs hospital and associated clinics.
Patients.There were 390 patients with MSSA infections and 335 patients with MRSA infections.
Methods.We used medical records, accounting systems, and interviews to identify services rendered and costs for Minneapolis Veterans Affairs Medical Center patients with S. aureus infection with onset during the period from January 1, 2004, through June 30, 2006. We used regression analysis to adjust for patient characteristics.
Results.Median 6-month unadjusted costs for patients infected with MRSA were $34,657, compared with $15,923 for patients infected with MSSA. Patients with MRSA infection had more comorbidities than patients with MSSA infection (mean Charlson index 4.3 vs 3.2; P < .001). For patients with Charlson indices of 3 or less, mean adjusted 6-month costs derived from multivariate analysis were $51,252 (95% CI, $46,041–$56,464) for MRSA infection and $30,158 (95% CI, $27,092–$33,225) for MSSA infection. For patients with Charlson indices of 4 or more, mean adjusted costs were $84,436 (95% CI, $79,843–$89,029) for MRSA infection and $59,245 (95% CI, $56,016–$62,473) for MSSA infection. Patients with MRSA infection were also more likely to die than were patients with MSSA infection (23.6% vs 11.5%; P < .001). MRSA infection was more likely to involve the lungs, bloodstream, and urinary tract, while MSSA infection was more likely to involve bones or joints; eyes, ears, nose, or throat; surgical sites; and skin or soft tissue (P < .001).
Conclusions.Resistance to methicillin in S. aureus was independently associated with increased costs. Effective antimicrobial stewardship and infection prevention programs are needed to prevent these costly infections.





